If you run a medical practice, you’ve probably told yourself your in-house billing setup costs roughly what you pay your biller somewhere around $45,000 to $55,000 a year.
Here’s the problem: that number is almost always wrong.
When every real cost is counted benefits, software, training, turnover, downtime, and lost revenue from claim errors — most practices are spending $90,000 to $140,000 per biller annually. And many don’t realize it until they finally run the numbers.
This guide does exactly that. At Rapid Claim Care, we’ve worked with hundreds of practices and seen this gap play out over and over. We break down the true cost of in-house billing versus a professional billing service so you can make a clear, informed decision for your practice in 2026.
The Hidden Cost Problem With In-House Billing
Most practice owners calculate billing cost as: salary + software = total.
That’s not even close to the full picture. Here’s what actually goes into keeping a biller on payroll.
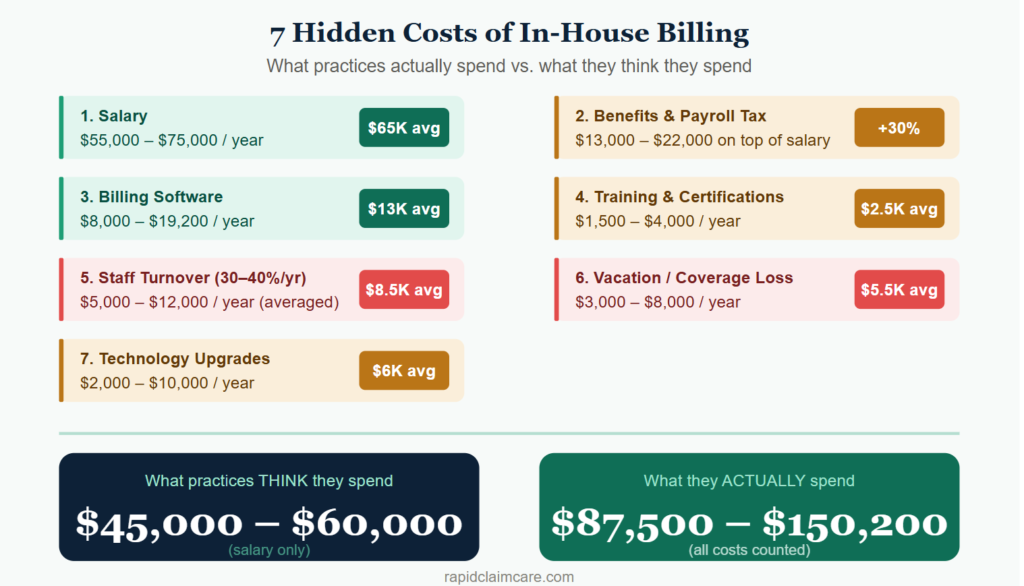
Full In-House Billing Cost Breakdown (Per Biller, Per Year)
1. Salary
In 2026, a medical biller earns between $55,000 and $75,000 annually depending on experience, specialty knowledge, and location. In major metro areas, experienced billers command the higher end of that range. Coding specialists earn even more typically $50,000 to $75,000.
Annual cost: $55,000 – $75,000
2. Benefits and Payroll Taxes
This is where most practices dramatically underestimate their costs. Benefits add 25–40% on top of base salary, including:
- Payroll taxes (7.65% employer share)
- Health insurance: $8,000 – $15,000 per employee
- 401(k) match: 3–5% of salary
- Paid time off (15–20 days = roughly $3,000–$6,000 in lost productivity)
- Workers’ compensation insurance
A biller earning $55,000 costs your practice $68,000–$77,000 before they’ve submitted a single claim.
Annual cost: $13,000 – $22,000 on top of salary
3. Billing Software
Your practice needs practice management software with robust billing capabilities. In 2026, this runs $300–$800 per month per provider, plus clearinghouse fees, electronic remittance fees, and any add-ons for eligibility verification or denial tracking.
For a 2-provider practice, that’s easily $8,000–$19,200 per year just for software your biller needs to do their job.
Annual cost: $8,000 – $19,200
4. Training and Continuing Education
Medical billing codes, payer rules, and compliance requirements change every year. ICD-10 updates, CPT code revisions, Medicare fee schedule changes a good biller must stay current. Certifications, webinars, and industry courses cost money and time.
Annual cost: $1,500 – $4,000
5. Turnover — The Cost Nobody Talks About
Medical billing has one of the highest turnover rates in healthcare administration — 30–40% annually. Every time a biller leaves, your practice faces:
- 2–3 months of reduced productivity while the backlog builds
- 1–2 months of recruiting and interviewing
- 3–4 months before a new hire reaches full speed
- Job board fees, HR time, and onboarding costs
For a position paying $55,000, total turnover cost runs $15,000–$25,000 each time. If your biller leaves every 2–3 years, that’s $5,000–$12,000 per year in hidden costs not counting the revenue lost during the gap.
Annual cost: $5,000 – $12,000 (averaged)
6. Vacation and Sick Day Coverage
When your biller takes two weeks off, who submits claims? In most small practices, the answer is: nobody. Claims pile up, cash flow stalls, and you’re paying a full salary for zero billing output during that period.
Practices with only one or two billing staff have zero redundancy. Any absence directly hits revenue.
Annual revenue impact: $3,000 – $8,000
7. Technology Upgrades
Billing software doesn’t stay current forever. Periodic system upgrades, data migrations, and staff retraining on new platforms happen every 3–5 years — costing $10,000–$30,000 per overhaul, or roughly $2,000–$10,000 annually when averaged out.
Annual cost: $2,000 – $10,000
True In-House Total: What You’re Really Spending
| Cost Category | Low Estimate | High Estimate |
|---|---|---|
| Salary | $55,000 | $75,000 |
| Benefits & Payroll Taxes | $13,000 | $22,000 |
| Billing Software | $8,000 | $19,200 |
| Training & Certifications | $1,500 | $4,000 |
| Turnover (averaged) | $5,000 | $12,000 |
| Vacation/Coverage Loss | $3,000 | $8,000 |
| Technology Upgrades | $2,000 | $10,000 |
| Total Per Biller/Year | $87,500 | $150,200 |
For a small practice billing under $3 million annually, in-house billing typically costs $90,000–$140,000 per biller per year when all true costs are counted. Most practices estimate $45,000–$60,000. The gap between what they think they’re spending and what they’re actually spending is the problem.
What a Professional Billing Service Actually Costs
Outsourced billing services use straightforward pricing. At Rapid Claim Care, we charge a simple percentage of net collections and that’s it. No hidden fees, no surprise software bills, no HR headaches. Most professional billing services charge 4–9% depending on specialty and claim volume.
| Practice Type | Monthly Collections | Service Fee (6%) | Annual Cost |
|---|---|---|---|
| Solo primary care | $80,000 | $4,800/mo | $57,600 |
| 2-provider practice | $150,000 | $9,000/mo | $108,000 |
| 3-provider specialty | $250,000 | $15,000/mo | $180,000 |
For simple specialties like primary care or family medicine, rates typically fall in the 4–6% range. High-complexity specialties such as neurology, oncology, or pain management run 7–9% due to greater prior authorization and denial management requirements.
Some services charge a flat monthly fee instead — typically $1,500–$5,000/month for small practices.
Head-to-Head Comparison: Real Numbers
Let’s use a concrete example. A solo physician practice collecting $1,000,000 per year:
In-House Billing:
- Biller salary: $60,000
- Benefits (30%): $18,000
- Software: $12,000
- Training/turnover/coverage: $10,000
- Total: $100,000/year
Rapid Claim Care (6% service fee):
- Service fee: $60,000/year
- No software costs
- No benefits or HR overhead
- No turnover risk
- Total: $60,000/year
Savings from outsourcing: $40,000/year — on a $1M practice.
Now factor in that outsourced billing companies typically achieve clean claim rates of 95%+ versus 80–85% for average in-house teams. On $1,000,000 in collections, a 5% improvement in collections means $50,000 in additional recovered revenue.
Combined, many practices see $80,000–$100,000 in financial improvement in their first year after outsourcing.
What You Get With Rapid Claim Care (That You Don’t Get In-House)
Beyond the cost savings, partnering with Rapid Claim Care brings capabilities that are genuinely difficult to replicate in-house:
A full team, not one person. When you work with Rapid Claim Care, your claims never stop. Our team covers every shift, every absence there’s always a trained specialist handling your billing.
Specialty expertise. Rapid Claim Care works across dozens of specialties and payer contracts. We know denial patterns, appeal strategies, and payer-specific rules that a solo in-house biller may never encounter.
Technology included. Software, clearinghouse access, eligibility verification tools, and denial tracking are all included in your Rapid Claim Care service. You pay nothing extra.
Scalability. As your practice grows, Rapid Claim Care scales with you. No hiring, no retraining, no lag time.
Compliance coverage. HIPAA, ICD-10 updates, Medicare changes — Rapid Claim Care stays current so you don’t have to.
When In-House Billing Makes Sense
Outsourcing isn’t the right answer for every practice. In-house billing can still make sense if:
- You bill over $5 million annually and have enough volume to support a full internal team with redundancy
- Your specialty has highly unique documentation requirements that benefit from embedded staff
- You have a dedicated billing manager with strong oversight systems already in place
- You run a large group practice where the per-provider cost of outsourcing exceeds in-house costs at scale
For the majority of practices — especially those with fewer than 10 physicians or billing under $3 million annually — the math strongly favors outsourcing once all real costs are counted.
Questions to Ask Before You Decide
If you’re still on the fence, answer these honestly:
- Do you know your current clean claim rate?
- What is your denial rate, and how quickly are denials appealed?
- What happens to billing when your biller is sick or on vacation?
- How long does it currently take to collect on a submitted claim?
- Have you ever calculated your total billing cost including all the categories above?
If any of these questions are hard to answer, that’s information in itself.
The Bottom Line
The real cost of an in-house medical biller in 2026 is not the salary you see on your payroll report. It’s the full stack: salary, benefits, software, training, turnover, downtime, and the revenue lost to claim errors and denials.
For most practices, partnering with Rapid Claim Care costs significantly less than in-house billing while delivering better collections, faster reimbursements, and zero staffing headaches.
The question is no longer whether outsourcing costs less. For most practices, it clearly does. The question is how much revenue your current setup is costing you — and how long you’re willing to wait to fix it.
Ready to see what your practice could save with Rapid Claim Care?
Contact us today for a free billing audit. Our team will analyze your current collections, denial rate, and true billing costs and show you exactly what partnering with Rapid Claim Care would mean for your bottom line.
Get Your Free Billing Audit from Rapid Claim Care →

